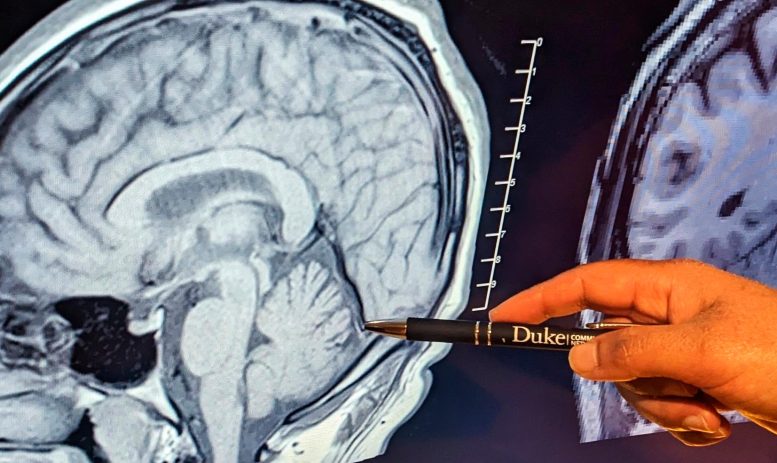
The cerebellum, indicated by pointer, is the brain within the brain or the tiny brain. It contains half of the brain’s neurons, tightly packed. New research shows that PTSD is associated with a smaller cerebellum, offering new insights into the neurological underpinnings of the disorder and potential treatment approaches. Credit: Dan Vahaba, Duke University
People with larger data-sharing initiative, pooled together their brain imaging scans to study PTSD as broadly and universally as possible.
The group ended up with images from 4,215 adult MRI scans, about a third of whom had been diagnosed with PTSD.
“I spent a lot of time looking at cerebellums,” Huggins said.
Even with automated software to analyze the thousands of brain scans, Huggins manually spot-checked every image to make sure the boundaries drawn around the cerebellum and its many subregions were accurate.
The result of this thorough methodology was a fairly simple and consistent finding: PTSD patients had cerebellums about 2% smaller.
When Huggins zoomed in to specific areas within the cerebellum that influence emotion and memory, she found similar cerebellar reductions in people with PTSD.
Huggins also discovered that the worse PTSD was for a person, the smaller their cerebellum was.
“Focusing purely on a yes-or-no categorical diagnosis doesn’t always give us the clearest picture,” Huggins said. “When we looked at PTSD severity, people who had more severe forms of the disorder had an even smaller cerebellar volume.”
Targeting the Cerebellum for Treatment and More Research
The results are an important first step in looking at how and where PTSD affects the brain.
There are more than 600,000 combinations of symptoms that can lead to a PTSD diagnosis, Huggins explained. Figuring out if different PTSD symptom combinations have different impacts on the brain will also be important to keep in mind.
For now, though, Huggins hopes this work helps others recognize the cerebellum as an important driver of complex behavior and processes beyond gait and balance, as well as a potential target for new and current treatments for people with PTSD.
“While there are good treatments that work for people with PTSD, we know they don’t work for everyone,” Huggins said. “If we can better understand what’s going on in the brain, then we can try to incorporate that information to come up with more effective treatments that are longer lasting and work for more people.”
Reference: “Smaller total and subregional cerebellar volumes in posttraumatic stress disorder: a mega-analysis by the ENIGMA-PGC PTSD workgroup” by Ashley A. Huggins, C. Lexi Baird, Melvin Briggs, Sarah Laskowitz, Ahmed Hussain, Samar Fouda, Courtney Haswell, Delin Sun, Lauren E. Salminen, Neda Jahanshad, Sophia I. Thomopoulos, Dick J. Veltman, Jessie L. Frijling, Miranda Olff, Mirjam van Zuiden, Saskia B. J. Koch, Laura Nawjin, Li Wang, Ye Zhu, Gen Li, Dan J. Stein, Jonathan Ipser, Soraya Seedat, Stefan du Plessis, Leigh L. van den Heuvel, Benjamin Suarez-Jimenez, Xi Zhu, Yoojean Kim, Xiaofu He, Sigal Zilcha-Mano, Amit Lazarov, Yuval Neria, Jennifer S. Stevens, Kerry J. Ressler, Tanja Jovanovic, Sanne J. H. van Rooij, Negar Fani, Anna R. Hudson, Sven C. Mueller, Anika Sierk, Antje Manthey, Henrik Walter, Judith K. Daniels, Christian Schmahl, Julia I. Herzog, Pavel Říha, Ivan Rektor, Lauren A. M. Lebois, Milissa L. Kaufman, Elizabeth A. Olson, Justin T. Baker, Isabelle M. Rosso, Anthony P. King, Isreal Liberzon, Mike Angstadt, Nicholas D. Davenport, Scott R. Sponheim, Seth G. Disner, Thomas Straube, David Hofmann, Rongfeng Qi, Guang Ming Lu, Lee A. Baugh, Gina L. Forster, Raluca M. Simons, Jeffrey S. Simons, Vincent A. Magnotta, Kelene A. Fercho, Adi Maron-Katz, Amit Etkin, Andrew S. Cotton, Erin N. O’Leary, Hong Xie, Xin Wang, Yann Quidé, Wissam El-Hage, Shmuel Lissek, Hannah Berg, Steven Bruce, Josh Cisler, Marisa Ross, Ryan J. Herringa, Daniel W. Grupe, Jack B. Nitschke, Richard J. Davidson, Christine L. Larson, Terri A. deRoon-DOI: 10.1038/s41380-023-02352-0


