A study reveals that midlife mortality rates in the US and UK are worsening compared to other high-income countries, with preventable causes such as drug overdoses driving this trend in the US. The UK faces similar challenges, particularly among younger women, indicating significant room for improvement in public health policies and interventions.
A new study by researchers at the Leverhulme Centre for Demographic Science (LCDS) and 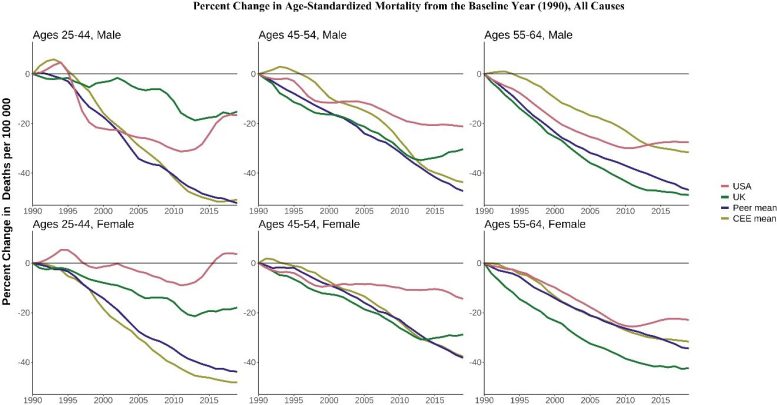
Age-standardized mortality from drug-related causes from 2000-2019. CEE, Central and Eastern European country. ‘Peer’ indicates a high-income country comparable to the USA. Credit: Oxford Population Health
Worsening midlife mortality in the US was driven by several causes of death, including highly preventable ones such as transport accidents, homicide, suicide, and drug overdoses. For example, drug-related deaths in the US increased up to 10-fold (depending on sex and age group combination) between 2000 and 2019, diverging tremendously from other countries.
Comparative Analysis and UK’s Position
Dr Katarzyna Doniec, corresponding author of the study and Postdoctoral Researcher at LCDS and the Demographic Science Unit said, ‘Over the past three decades midlife mortality in the US has worsened significantly compared to other high-income countries, and for the younger 25 to 44 year old age-group in 2019 it even surpassed midlife mortality rates for Central and Eastern European countries. This is surprising, given that not so long ago some of these countries experienced high levels of working-age mortality, resulting from the post-socialist crisis of the 1990s.’
The study highlights the health disadvantage of younger US females aged 25-44 years old who were the only group across the 25 countries studied to experience higher mortality rates in 2019 than in 1990.
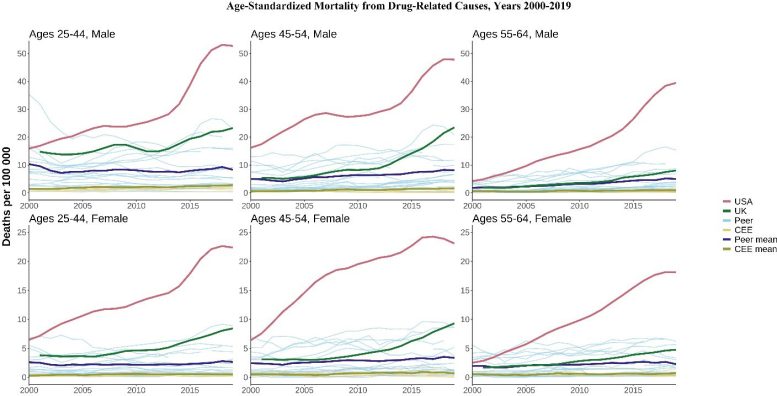
Percentage change in all-cause mortality rates since 1990. CEE, Central and Eastern European country. ‘Peer’ indicates a high-income country comparable to the USA. Credit: Oxford Population Health
The UK is also falling behind its high-income peers with midlife mortality increasing for people aged 45-54, and death rates among 25-54 year olds stagnating instead of improving. Midlife mortality among 25-44-year-olds also rose in Canada since 2013 alongside small increases for males of the same age range in Poland and Sweden, although these increases were far smaller than in the US.
While the UK performed relatively well on external causes of death such as suicide, homicide, and traffic accidents, this was countered by stalling improvements in when the life expectancy gap between the US and high-income countries widened further.
Reference: “US exceptionalism? International trends in midlife mortality” by Jennifer Beam Dowd, Katarzyna Doniec, Luyin Zhang and Andrea Tilstra, 21 March 2024, International Journal of Epidemiology.
DOI: 10.1093/ije/dyae024


